policy frameworks |
|
Information
Policy frameworks is a structure used to organise a set of principles and long term goals which include rules, guidance and an overall direction for planning and development. Many are used in the health and social care sector to reduce inequality of care. Some also include the ways in which we can assess needs and how to decide whether a service user is eligible for help. They are used to ensure that service users challenges are minimised and they are at lower risk of experiencing these challenges.
For your assignment you need to understand what they mean, how they help minimise the challenges we have covered and how they may be used with the service users in your case studies.
Policy frameworks is a structure used to organise a set of principles and long term goals which include rules, guidance and an overall direction for planning and development. Many are used in the health and social care sector to reduce inequality of care. Some also include the ways in which we can assess needs and how to decide whether a service user is eligible for help. They are used to ensure that service users challenges are minimised and they are at lower risk of experiencing these challenges.
For your assignment you need to understand what they mean, how they help minimise the challenges we have covered and how they may be used with the service users in your case studies.
The role of policy frameworks in minimising challenges
> NHS Patient Experience Framework – including the eight elements
> Health Action Plans
> Adult Social Care Outcomes Framework (ASCOF)
> Common Assessment Framework (CAF)
> NHS Patient Experience Framework – including the eight elements
> Health Action Plans
> Adult Social Care Outcomes Framework (ASCOF)
> Common Assessment Framework (CAF)
NHS Patient Experience Framework
This sets out a definition of a positive patient experience built around the eight elements which make up good patient care.
1. Respect for patient centred values
2. Integration of care across the HSC system
3. Information and communication on clinical status
4. Physical comfort
5. Emotional support
6. Involvement of family and friends
7. Transition of care outside of HSC setting
8. Access to care – wait times
This sets out a definition of a positive patient experience built around the eight elements which make up good patient care.
1. Respect for patient centred values
2. Integration of care across the HSC system
3. Information and communication on clinical status
4. Physical comfort
5. Emotional support
6. Involvement of family and friends
7. Transition of care outside of HSC setting
8. Access to care – wait times
|
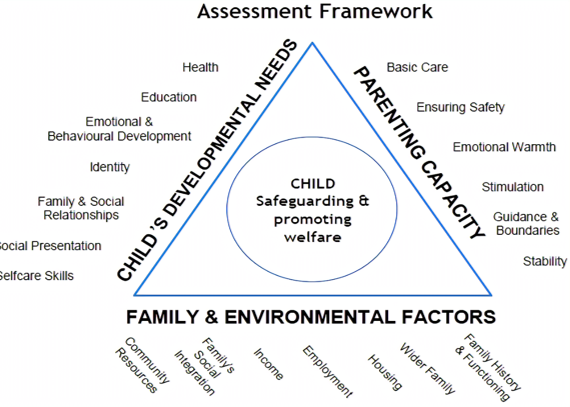
Common Assessment Framework (CAF)
> Pre assessment checklist > It will help identify any problems or concerns > Aims to give early intervention before problems get worse > Parent and/or child have to give permission as it is a voluntary assessment > Have needs in one or more of the three areas on the sides of the triangle |
Health actions plans
The plans aim to minimise challenges by looking at what pressures the services may face.
> Pressures are:
The plans aim to minimise challenges by looking at what pressures the services may face.
> Pressures are:
- Ageing society
- Long term conditions e.g. dementia
- Increase in our expectations of the health service
Adult Social Care Outcomes Framework (ASCOF)
> (2011)
> Measures performance of services against the aim of ensuring the most vulnerable people receive high quality care regardless of where they live.
> It covers the following
> Enhancing quality of life for people with care and support needs
> Reducing the need for care and support
> Positive experiences of care and support
> Safeguarding adults that are vulnerable
> Yearly reports for each local authority are given on this
> This will help overcome challenges because it should provide support for all individuals regardless of who they are and where they live.
> (2011)
> Measures performance of services against the aim of ensuring the most vulnerable people receive high quality care regardless of where they live.
> It covers the following
> Enhancing quality of life for people with care and support needs
> Reducing the need for care and support
> Positive experiences of care and support
> Safeguarding adults that are vulnerable
> Yearly reports for each local authority are given on this
> This will help overcome challenges because it should provide support for all individuals regardless of who they are and where they live.
Impact of not enabling individuals to overcome challenges
It is difficult to ensure that all service providers know about the latest guidance in their particular field of care, what needs to change as a result of it and be motivated or accepting enough to make changes. Sometimes there are several sets of guidance coming from different bodies, which can make it hard to get service providers and users to engage wit the guidance. If service providers don’t make the changes, then service users aren’t able to make the changes necessary to improve their health and wellbeing. A challenge, such as the ageing population not being effectively tackled, could become a crisis in the future. The NHS could reach breaking point because it has reached its capacity, and the environments such as care homes may have to turn people away. Services and outcomes for service users wont improve, and early identification and intervention wont happen, which leads to a greater need for specialist services.
It is difficult to ensure that all service providers know about the latest guidance in their particular field of care, what needs to change as a result of it and be motivated or accepting enough to make changes. Sometimes there are several sets of guidance coming from different bodies, which can make it hard to get service providers and users to engage wit the guidance. If service providers don’t make the changes, then service users aren’t able to make the changes necessary to improve their health and wellbeing. A challenge, such as the ageing population not being effectively tackled, could become a crisis in the future. The NHS could reach breaking point because it has reached its capacity, and the environments such as care homes may have to turn people away. Services and outcomes for service users wont improve, and early identification and intervention wont happen, which leads to a greater need for specialist services.